Pneumonia
 Called an Iron Lung, the negative pressure ventilator was a common tool used to treat polio when that disease was deadly and much feared. Poliomyelitis, which is often called polio or infantile paralysis, is an infectious disease caused by the poliovirus. In about 0.5 percent of cases there is muscle weakness resulting in an inability to move. This can occur over a few hours to a few days. The weakness most often involves the legs but may less commonly involve the muscles of the head, neck and diaphragm. Many people fully recover. In those with muscle weakness about 2 to 5 percent of children and 15 to 30 percent of adults die. Another 25 percent of people have minor symptoms such as fever and a sore throat and up to 5 percent have headache, neck stiffness and pains in the arms and legs. These people are usually back to normal within one or two weeks. In up to 70 percent of infections there are no symptoms. Years after recovery post-
Called an Iron Lung, the negative pressure ventilator was a common tool used to treat polio when that disease was deadly and much feared. Poliomyelitis, which is often called polio or infantile paralysis, is an infectious disease caused by the poliovirus. In about 0.5 percent of cases there is muscle weakness resulting in an inability to move. This can occur over a few hours to a few days. The weakness most often involves the legs but may less commonly involve the muscles of the head, neck and diaphragm. Many people fully recover. In those with muscle weakness about 2 to 5 percent of children and 15 to 30 percent of adults die. Another 25 percent of people have minor symptoms such as fever and a sore throat and up to 5 percent have headache, neck stiffness and pains in the arms and legs. These people are usually back to normal within one or two weeks. In up to 70 percent of infections there are no symptoms. Years after recovery post-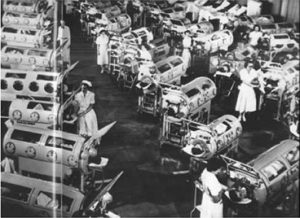 polio syndrome may occur, with a slow development of muscle weakness similar to that experienced during the initial infection. Polio is more common in infants and young children, occurring under conditions of poor hygiene.
polio syndrome may occur, with a slow development of muscle weakness similar to that experienced during the initial infection. Polio is more common in infants and young children, occurring under conditions of poor hygiene.
Because of complete or partial loss of muscle usage, people with polio had a difficult time breathing, which can cause a myriad of problems, including pneumonia. Enter the Emerson iron lung. The affected patient lies within the chamber, which when sealed provides an effectively oscillating atmospheric pressure. A negative pressure ventilator, or iron lung, is a nearly-obsolete mechanical respirator which enables a person to breathe on their own in a normal manner, when muscle control is lost, or the work of breathing exceeds the person’s ability, as may result from certain diseases. Polio was not the only disease that called for the iron lung. In addition to  Polio, botulism and certain poisons, such as barbiturates, tubocurarine, also benefited from its use.
Polio, botulism and certain poisons, such as barbiturates, tubocurarine, also benefited from its use.
Versions of the Iron Lung include both the Drinker respirator, the Emerson respirator, and the Both (Emerson-Drinker) respirator. The negative form of pressure ventilation…decreasing surrounding pressure to induce inhalation then re-pressurizing to 1 bar (15 psi; 750 mmHg)…has been almost entirely superseded by positive pressure ventilation (forcing air into the lungs with a pressure greater than 1 bar then allowing the body to naturally exhale before repeating) or negative pressure cuirass ventilation. While the iron lung is not used anymore, it served a useful purpose in its day.
 Whenever we make a trip to the emergency room, most of us find ourselves waiting impatiently for the myriad of tests to be returned from the lab to find out what is going on. And, most of us find that annoying, but when you think about how things used to be diagnosed, you might just find yourself rethinking those tests. Imagine a time when something like Pneumonia, Bronchitis, or Tuberculosis might have been “diagnosed” by having you doctor place his ear to your chest to see what you sound like. While I’m no expert, I have a pretty good idea that those three lung diseases would sound fairly similar. So if you had Tuberculosis and your doctor treated you for Bronchitis, how good would you expect your prognosis to be. Not very good, but this was all the doctor could do at that time.
Whenever we make a trip to the emergency room, most of us find ourselves waiting impatiently for the myriad of tests to be returned from the lab to find out what is going on. And, most of us find that annoying, but when you think about how things used to be diagnosed, you might just find yourself rethinking those tests. Imagine a time when something like Pneumonia, Bronchitis, or Tuberculosis might have been “diagnosed” by having you doctor place his ear to your chest to see what you sound like. While I’m no expert, I have a pretty good idea that those three lung diseases would sound fairly similar. So if you had Tuberculosis and your doctor treated you for Bronchitis, how good would you expect your prognosis to be. Not very good, but this was all the doctor could do at that time.
Enter René Théophile Hyacinthe Laennec (February 17, 1781 – August 13, 1826), a young man who’s mother died of tuberculosis when he was five years old. Laennec went to live with his great uncle the Abbé Laennec, who was a priest. As a child, Laennec became ill with Lassitude and repeated instances of Pyrexia. Laennec was also thought to have Asthma. At the age of twelve, he proceeded to Nantes, where his uncle, Guillaime-François Laennec, worked in the faculty of medicine at the university. Laennec was a gifted student. He learned English and German and began his medical studies under his uncle’s direction. Laennec knew first hand that  things like Tuberculosis can kill…he lived that nightmare with his mom. I am fairly certain that there were probably issues with her diagnosis too. After studying medicine, Laennec became a doctor. He also became a lecturer at the Collège de France in 1822 and professor of medicine in 1823. His final appointments were that of head of the medical clinic at the Hôpital de la Charité and professor at the Collège de France.
things like Tuberculosis can kill…he lived that nightmare with his mom. I am fairly certain that there were probably issues with her diagnosis too. After studying medicine, Laennec became a doctor. He also became a lecturer at the Collège de France in 1822 and professor of medicine in 1823. His final appointments were that of head of the medical clinic at the Hôpital de la Charité and professor at the Collège de France.
Laennec’s father was a lawyer, and he thought that being a doctor was a waste of René’s talents. With his father’s discouragement, René had a period of time during which he took long walks in the country, danced, studied Greek and wrote poetry. However, in 1799 he returned to study. Laennec studied medicine at the University of Paris under several famous physicians, including Dupuytren and Jean-Nicolas Corvisart-Desmarets. There he was trained to use sound as a diagnostic aid. Corvisart advocated the re-introduction of percussion during the French Revolution. In 1816, he was consulted by a young woman laboring under general symptoms of diseased heart, and in whose case percussion and the application of the hand were of little avail on account of the great degree of fatness. “The other method just mentioned [direct auscultation] being rendered inadmissible by the age and sex of the patient, I happened to recollect a simple and well-known fact, in acoustics…the great distinctness with which we hear the scratch of a pin at one end of a piece of wood on  applying our ear to the other. Immediately, on this suggestion, I rolled a quire of paper into a kind of cylinder and applied one end of it to the region of the heart and the other to my ear, and was not a little surprised and pleased to find that I could thereby perceive the action of the heart in a manner much more clear and distinct than I had ever been able to do by the immediate application of my ear.” This situation started Laennec’s mind whirling, and before long, he had developed a simplistic version of what we now are all very familiar…the stethoscope. Ironically, like his mother, Laennec died of Tuberculosis on August 13, 1826. While I’m sure medicine had vastly improved during his lifetime, there was still no significant help for Tuberculosis.
applying our ear to the other. Immediately, on this suggestion, I rolled a quire of paper into a kind of cylinder and applied one end of it to the region of the heart and the other to my ear, and was not a little surprised and pleased to find that I could thereby perceive the action of the heart in a manner much more clear and distinct than I had ever been able to do by the immediate application of my ear.” This situation started Laennec’s mind whirling, and before long, he had developed a simplistic version of what we now are all very familiar…the stethoscope. Ironically, like his mother, Laennec died of Tuberculosis on August 13, 1826. While I’m sure medicine had vastly improved during his lifetime, there was still no significant help for Tuberculosis.
 When we think of the president of the United States…in general terms, we often wonder if he will be good enough to be re-elected and serve the maximum term of eight years. We seldom think about whether or not he will finish his first year…or even month for that matter. And few of us can name the president with the sad title of being the president of the United States for the shortest term. Nevertheless, that is a record that has to be held by someone, and that man was William Henry Harrison, who was our 9th President. Harrison’s inaugural speech, delivered on a bitterly cold March morning, lasted one hour and forty five minutes. Harrison wasn’t really feeling well at the time, and went to bed at the end of inauguration day with a bad cold. The cold quickly developed into what would become a fatal case of pneumonia. I have to wonder if he would have been just fine in this day and age of modern medicine. Not everyone gets pneumonia these days, but most of those who do, survive and go on to lead long lives. Pneumonia isn’t the death sentence these days that it used to be.
When we think of the president of the United States…in general terms, we often wonder if he will be good enough to be re-elected and serve the maximum term of eight years. We seldom think about whether or not he will finish his first year…or even month for that matter. And few of us can name the president with the sad title of being the president of the United States for the shortest term. Nevertheless, that is a record that has to be held by someone, and that man was William Henry Harrison, who was our 9th President. Harrison’s inaugural speech, delivered on a bitterly cold March morning, lasted one hour and forty five minutes. Harrison wasn’t really feeling well at the time, and went to bed at the end of inauguration day with a bad cold. The cold quickly developed into what would become a fatal case of pneumonia. I have to wonder if he would have been just fine in this day and age of modern medicine. Not everyone gets pneumonia these days, but most of those who do, survive and go on to lead long lives. Pneumonia isn’t the death sentence these days that it used to be.
William Harrison was the last president born as an English subject before the American Revolution. After that time, it became law that the president must be a natural born citizen, something that has sparked bitter battles in these modern times. He hailed from Virginia, and attended college intending to become a doctor, but opted to join the army before finishing his degree. President John Adams took note of Harrison’s exemplary service in the Indian Wars of the Northwest Territories. In 1801, President Adams appointed him governor of the Northwest Territories, which is now Indiana and Illinois. Harrison later fought in the Battle of the Thames River during the War of 1812. After that time, he decided to go into politics, and went on to become a congressman and the ambassador to Colombia before running with John Tyler on the Whig Party ticket in the presidential election of 1840, which he won, but this would not prove to be a long term in office for him. In fact, his death came exactly one month after he was inaugerated into office.
I have to wonder what things he might have done differently than his running mate, John Tyler did. Harrison was 68 years and 23 days old when he took office. He was the oldest president to take office until Ronald  Reagan in 1981. After his passing, there was a brief constitutional crisis, because this had never happened before, and it had to be decided, who would take over. The solution was not widely accepted, and there were disputes as to the presidential line of succession, with regard to the Constitution up until the passage of the 25th Amendment in 1967. William Henry Harrison was the grandfather of Benjamin Harrison, who was the 23rd President from 1889 to 1893, so his line did have a second chance at the course that the country would take, even though he was not directly involved. Of course, there is nothing to indicate that Benjamin would have had the same values as William did. Things change over the years, but he was a Republican…a good thing in my opinion.
Reagan in 1981. After his passing, there was a brief constitutional crisis, because this had never happened before, and it had to be decided, who would take over. The solution was not widely accepted, and there were disputes as to the presidential line of succession, with regard to the Constitution up until the passage of the 25th Amendment in 1967. William Henry Harrison was the grandfather of Benjamin Harrison, who was the 23rd President from 1889 to 1893, so his line did have a second chance at the course that the country would take, even though he was not directly involved. Of course, there is nothing to indicate that Benjamin would have had the same values as William did. Things change over the years, but he was a Republican…a good thing in my opinion.
 In March of this year, my mother-in-law was in the hospital twice. The second hospital stay was followed by a little more than a two week stay in a nursing home…supposedly for rehab/physical therapy. That stay in a skilled nursing facility nearly killed her. After taking her out of the nursing home, she would have two more hospital stays. After the first one, they wanted to put her in a skilled nursing facility. After I told them about the horrible care she received and what we could do for her, her case worker agreed that we could do a better job of caring for her than any nursing facility could. Now I know that you are thinking you might be reading the first negative post from me, but that is as far from the truth as it gets.
In March of this year, my mother-in-law was in the hospital twice. The second hospital stay was followed by a little more than a two week stay in a nursing home…supposedly for rehab/physical therapy. That stay in a skilled nursing facility nearly killed her. After taking her out of the nursing home, she would have two more hospital stays. After the first one, they wanted to put her in a skilled nursing facility. After I told them about the horrible care she received and what we could do for her, her case worker agreed that we could do a better job of caring for her than any nursing facility could. Now I know that you are thinking you might be reading the first negative post from me, but that is as far from the truth as it gets.
Yes, my mother-in-law has been very sick and even close to death a couple of times, but as of this writing, she is doing well. I have been so pleased with her progress. She has Alzheimer’s Disease, as most of you know, and she doesn’t always understand the importance of some of the things she needs to do to recover, like wearing oxygen and walking to get stronger. She also doesn’t understand why she feels so weak…mostly because she doesn’t know that she had Bronchitis twice, Pneumonia twice, and Pleurisy twice since February 21st.
Today my mother-in-law was such a trooper. I have been making her get up and move 4 times a day…with the help of my wonderful husband, daughters, sister-in-law, and father-in-law. She didn’t want to do it, and sometimes we had to make her do it. She is one big sore muscle, truth be told. Even with all that, today that sweet woman who has been through so much over the last 2 1/2 months, got up every time I asked her to, walked further than she had in 2 months, cleaned up her plate at each meal (she hasn’t had much appetite in the last two months either), smiled like she used to, and talked with my father-in-law (another thing she hasn’t done much of lately). She worked so hard, through the pain and shortness of breath. I was so proud of her for all her hard work.
The last 2 1/2 months have been long and hard on her, but she is a fighter, and I know she has it in her to come back from this. We will not give up, and I will fight hard to keep her out of a nursing home, because she deserves every opportunity to live at home for as long as possible. Now, as I write this I hear from my daughter that she fought her so hard tonight that she had to have her husband come to help make her get up for bed…aw well, tomorrow is another day.
 Sometimes…when we least expect it, or maybe when we just weren’t looking, it occurs to us that those we love are getting older. Little problems begin to present themselves, that throw us for a loop. We begin to wonder how we could have missed the fact that someone is really in their early 80’s. I mean, we know their chronological age very well, but somehow their physical age sneaks up on us, and takes us very much by surprise.
Sometimes…when we least expect it, or maybe when we just weren’t looking, it occurs to us that those we love are getting older. Little problems begin to present themselves, that throw us for a loop. We begin to wonder how we could have missed the fact that someone is really in their early 80’s. I mean, we know their chronological age very well, but somehow their physical age sneaks up on us, and takes us very much by surprise.
That is exactly what happened to me last Monday, with my father-in-law, and we spent the rest of the week with him in the hospital, while we waited to see if the racing heart rate that his foot doctor caught was going to be problematic, or just a result of the Pneumonia that he was also diagnosed with. Like my own dad, my father-in-law had always seemed much younger that his years, so suddenly being faced with something that could be a life or death situation, just about knocked me over, as did the possibility of losing the first line caregiver for my mother-in-law.
The diagnosis came, and we will be dealing with A-Fib for the rest of his life, but since my mom has that, I know it is manageable. The Pneumonia is pretty much gone, and he came home from the hospital today. He would like to think that he can just go back to life as usual, but for me, much has changed. Yes, he was on oxygen before, and weak in that way, but the rest of him was always strong and able to handle the majority of the care of my mother-in-law, but now…I have to consider that the stress of caring for an Alzheimer’s patient might be too much for him. Still, he has not come to a place where he is ready for her care to take a different turn, and we will honor his wishes concerning that decision. And, we aren’t ready for that change either.
So, we will modify the plan for now, until we know where we stand in this situation, and home health care will help with the day to day care for both of them. And we will see where the future will take us. In the case of my mom, the meds control her A-Fib quite well and she can do pretty much what she wants to. I pray that my father-in-law will be with be the same, and that the sudden changes that have come about will be able to return to at least some semblance of normalcy.

